May-Thurner Syndrome
A Hidden Condition That Can Go
Undetected Even With Advanced Imaging
What is May-Thurner Syndrome?
There are two main blood vessels in your legs – the iliac vein and iliac artery. May-Thurner Syndrome is a condition that causes the right iliac artery to press against the left iliac vein in the pelvis, narrowing the vessel. Often, there are no symptoms. The reduced blood flow can cause clots and Deep Vein Thrombosis (DVT).
Causes & Risk Factors
The primary cause of May-Thurner Syndrome is anatomical; the right iliac artery crosses over the left iliac vein, potentially compressing it. Certain factors might increase the risk, including: Prolonged periods of inactivity or immobilization. A history of vascular issues or clotting disorders. Hormonal factors, such as pregnancy or the use of birth control pills, which can increase blood clotting tendencies.
Diagnosis
Diagnosis of May-Thurner Syndrome typically involves imaging studies to view the blood vessels and assess any obstructions or compressions. These might include:
- Venography: A dye is injected into the veins to provide a clear view of the veins and any blockages.
- Ultrasound: Used to visualize blood flow and detect clots.
- CT or MRI scans: Provide detailed images of the vascular anatomy and can help identify the compression.
Treatment
The treatment for May-Thurner Syndrome focuses on managing symptoms and preventing complications, such as DVT. Treatment options may include:
- Blood thinners (anticoagulants) to prevent clot formation.
- Stenting to open up the compressed vein and restore normal blood flow.
- Compression stockings to help reduce swelling and improve blood flow.
For individuals diagnosed with May-Thurner Syndrome, ongoing monitoring and follow-up care with a vascular specialist are essential to manage the condition and prevent serious complications.
Symptoms of May-Thurner Syndrome
- Pain, swelling, tenderness
- Throbbing in the lower leg, usually worse on the left
- Potentially lower back pain
- Sensation of warmth
- Skin discoloration, especially at the ankles
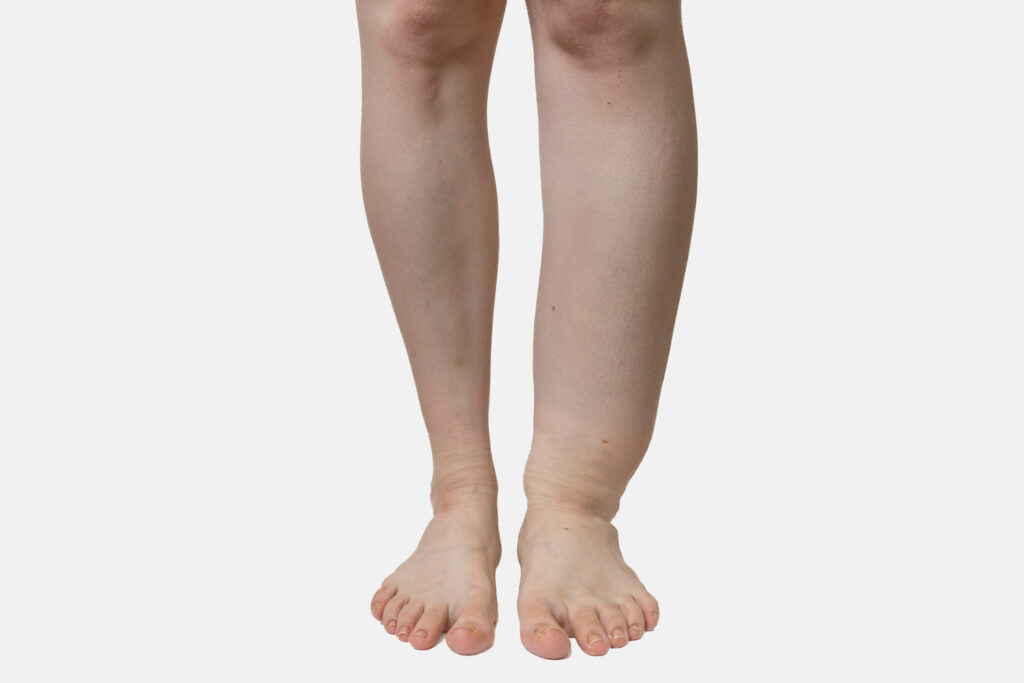
- One leg is larger than the other
- Varicose veins in the pelvic area
Symptoms of PTS
Fortunately, May-Thurner Syndrome is easy to treat. Using our intravascular ultrasound (IVUS), we locate the affected area, and insert a tiny balloon to open the vein and restore blood flow. We insert a small stent or metal mesh tube to keep it open.
Outcomes are excellent for this procedure, especially when performed early, before blood clots form.
Concerned You May Have May-Thurner Syndrome?
Many people don’t realize they have May-Thurner Syndrome until it leads to DVT. We can screen for DVT with an MRI or CT scan.
Get Treated Sooner
Because we’re highly specialized in treating May-Thurner Syndrome, with seven treatment locations in the St. Louis area, we’re able to schedule your exam and treatment much sooner than other facilities. Call us at 314-956-1818 or complete this contact form to get started.
Schedule a Consultation
What To Expect
Consultation
Dr. Krikorain will examine your legs and feet. We’ll provide shorts to wear during the exam, if needed. You may have an ultrasound, also known as a VRS (venous reflux study), and we may schedule you for further testing.
Procedures
Treatment for May-Thurner Syndrome will be stent placement at one of our outpatient surgery centers.
Recovery
You will have 3-5 days of lifting restrictions, and we’ll prescribe a blood thinner short term.

"No More Pain"
MaryAnn R.

"I Walked 2 Miles the Next Day!"
Shirley M.

"They Listen Very Well!"
Jeff K.

"Very Knowledgable!"
Happy Patient

"My Leg is Feeling So Much Better!"
Marlene G.
May-Thurner Syndrome FAQ
You are most at risk if you’re female, between the ages of 24-40. If you’ve recently given birth, especially to twins or more, or are on oral contraceptives, you have an elevated risk. Other risks include dehydration, hypercoagulable disorders, and cumulative radiation exposure.
This is a medical condition, so most insurances cover treatment.
If you get a stent, you may have low back or hip pain for 2-3 weeks following the procedure.
This syndrome/symptoms of this syndrome may return if there is re-narrowing of the stent or if there is medication noncompliance.
No, unfortunately, this condition is genetic.

